If your teen is suddenly complaining about soreness in the back of their mouth, or their dentist starts bringing up “those third molars,” you’re probably wondering:
If wisdom teeth cause so many problems… why do we even have them?
Fair question — and the answer goes way back.
A Throwback From Our Caveman Days
Wisdom teeth are basically nature’s leftovers. Our ancestors ate tough, raw foods that required major chewing power. Their jaws were bigger, broader, and built to handle it, so having an extra set of molars was an advantage.
Fast-forward to today:
- Our diets are softer
- Our jaws are smaller
- And these third molars often have nowhere to go
That’s why so many teens and young adults experience issues like crowding, pain, infections, or impacted wisdom teeth that never fully break through the gums.
Why Monitoring Wisdom Teeth Matters
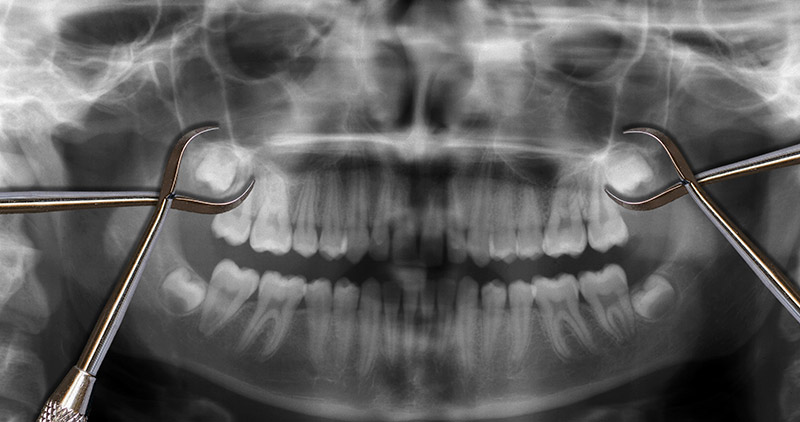
Most wisdom teeth start making their appearance between ages 15–25. Regular checkups — especially digital X-rays — help us track how these molars are forming, the direction they’re growing, and whether they’ll cause trouble.
Your teen’s dentist may recommend removing them if they’re:
- Growing sideways
- Stuck under the gum or bone
- Crowding other teeth
- Causing pain, swelling, or infection
- At risk of damaging nearby teeth
And that’s where we come in.
Expert, Comfortable Wisdom Tooth Removal at CT Maxillofacial Surgeons
When it’s time to talk wisdom teeth, your family wants a team that treats your teen like one of their own. Our surgeons specialize in safe, efficient wisdom tooth removal — with options like IV sedation to keep the experience calm, smooth, and stress-free.
We walk both patients and parents through the process step-by-step, so you always know what’s happening and what to expect during recovery.
Let’s Keep Your Teen’s Smile Healthy
If your dentist has recommended wisdom tooth evaluation or removal, we’re ready when you are.
CT Maxillofacial Surgeons is here to make the process simple, safe, and comfortable — start to finish.
Call us today to schedule a consultation

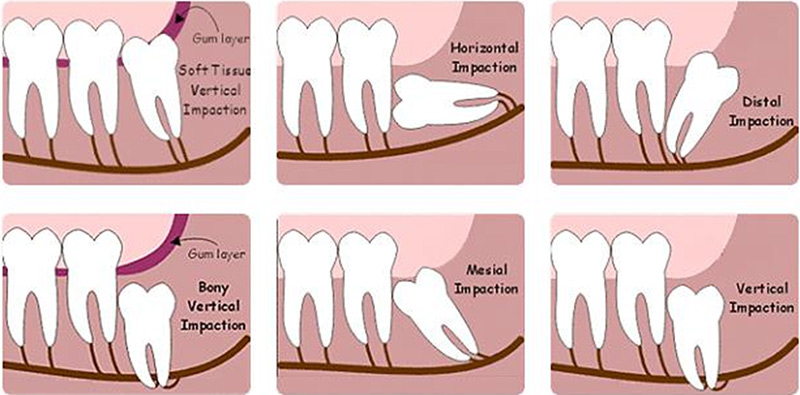 Wisdom teeth are the last molars to develop, usually between ages 17–25. While some people have no issues, most of us simply don’t have the space for them. That’s when problems like crowding, pain, or infection can occur.
Wisdom teeth are the last molars to develop, usually between ages 17–25. While some people have no issues, most of us simply don’t have the space for them. That’s when problems like crowding, pain, or infection can occur.